Stay ahead of the curve as a political insider with deep policy analysis, daily briefings and policy-shaping tools.
Request a Demo‘Completely dysfunctional’: How public health funding disparities are causing dangerous inequities in care


When an HIV outbreak threatened a rural community in Scott County in late 2014, the county near the Kentucky border was thrust into a political and moral debate over whether syringe exchanges were an appropriate way to handle a dangerous outbreak caused by intravenous drug use.
But, the outbreak also uncovered what should have been a less controversial problem in the county: A lack of HIV testing.
At the time, Scott County’s health department, operating on a shoe-string budget with only five full time employees, did not offer such testing, and the local Planned Parenthood in the area that previously did so closed in 2013.
Had there been earlier testing — and an earlier response — to the HIV outbreak in Scott County, a 2018 study from two Yale University professors found, there could have been just 10 infections.
Or fewer.
Instead, hundreds of infections were attributed to the outbreak that rocked the Austin, Indiana, community of just 4,000, the largest HIV outbreak seen in Indiana history.
“It was just kind of a perfect storm of a lot of things. There wasn’t any free prevention testing going on,” said Michelle Matern, the Scott County Health Department administrator. “And then there was a lack of health education.”
The outbreak in Austin, as well as the more recent COVID-19 pandemic, demonstrates the necessity of public health departments and the services they could be providing if properly funded.
Before the pandemic, Indiana only spent $55 per capita on public funding, compared to the U.S. average of $91, according to a report from the Governor’s Public Health . In fact, of the health departments that provided data, all but four reported revenues beneath the national 25th percentile in local health department funding.
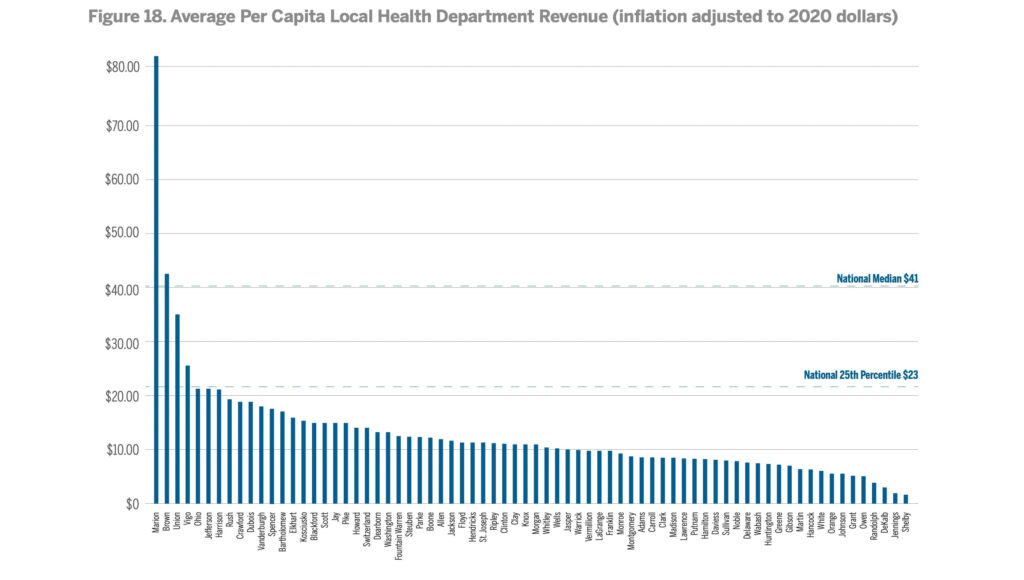
That matters in a state falling behind on nearly all health metrics, from obesity to early adult mortality. Perhaps the most important metric of all: Indiana ranked 40th in life expectancy in 2018, nearly two years below the U.S. rate. And the gap between the Hoosier state and the U.S. on that measure is only getting worse.
The Governor's Public Health Commission issued a report this summer making 32 recommendations to fix the public health funding problem, including a whopping $243 million increase in state funding per year to help rightsize public health departments.
That would be just enough to put Indiana at the average per capita funding for public health departments in the U.S. But getting state lawmakers — most of whom have no health expertise themselves — to commit to that level of funding when they return to the Statehouse in January is a tall order.
If you ask Indiana State Health Commissioner Dr. Kristina Box, it’s time for that investment in order to ensure care is equal across Indiana.
“Philosophically, I think it’s important that every Hoosier has access to having their best potential health,” she told State Affairs. “I’ve been an obstetrician and done deliveries for 30-plus years now, and I’ve never delivered a baby for a family that didn’t want the absolute best for that child.”
But health departments need to be able to play their part to ensure that’s possible, she said.
Disparities between counties
The stark reality of Indiana’s public health system is this: Where someone lives dictates the level of public health resources they have access to in a state with already inequitable health outcomes, in part because of how little funding the state itself contributes to the system.
“It shouldn’t matter where you live in the state of Indiana,” said Paul Halverson, dean of the Indiana University Richard M. Fairbanks School of Public Health. “Every resident of Indiana should be entitled to high quality public health services, because the reality is it’s not about the individual care, it’s about the care of the population.”
While the Marion County Health Department received $82.71 per resident in revenue, Shelby County received only $1.25 per resident in 2018, according to a 2020 Indiana Public Health System review from the Indiana University Richard M. Fairbanks School of Public Health.
The public, though, is often unaware of the wide-range of initiatives health departments touch, from food inspections to septic system reviews to disease and trauma prevention, which means the problem has gone unnoticed.
So what does the financial disparity mean in practice?
In a state that ranks 42 for smoking and tobacco use, only 15 county health departments, including the well-funded Marion County department, reported offering tobacco counseling services in 2021. More than 11,000 adult Hoosiers die each year due to smoking, according to the Campaign for Tobacco Free Kids.
Similarly, a child who lives in Vigo County, one of the top-four funded health departments in the state per the Fairbanks report, can get a physical at the child wellness clinic. In 2021, only four other counties reported providing any child well clinic services.

And in Vanderburgh County, which also has a better-funded department than most, the county engages with pregnant Hoosiers to provide wrap-around services for the first three years of their babies’ lives. Only eight other counties reported providing prenatal care services, despite Indiana’s status as the 9th worst state for infant mortality in 2020, according to the Centers for Disease Control.
Meanwhile, in 2021, at least 13 counties reported not providing blood lead screenings, despite the known health problems associated with lead exposure.
In fact, for years, the state health department didn’t follow Centers for Disease Control standards regarding when to investigate elevated blood levels in children. The reason: A lack of local health department funding and an unwillingness from state health leaders to implement another unfunded mandate that some local officials would just have to ignore.
The required basics aren’t necessarily being met in every county already. Box, the state health commissioner, said a local health department official told her they were responsible for emergency preparedness, food safety and septic systems. But because that employee was busy and didn’t really understand the food safety portion of the position, the county just wasn’t providing routine restaurant inspections.
Even in the larger Allen County Health Department, department administrator Mindy Waldron said it’s near impossible to focus on preventative measures, such as addressing the state’s dismal infant and maternal mortality rates or helping schools vaccinate children, when the county is already struggling to do the bare minimum required of it.
The department also has no trained epidemiologist, despite its status as the third largest health department in the state.
“We rob Peter to pay Paul every day to get to wherever we need to do these services,” Waldron said.
The lack of funding also means employees are spread thin. Waldron oversees the 66-person department, writes grants, works as a community health educator, completes half of the emergency preparedness planning and handles any human resources issues that may come up. She has no assistant, so when she has the day off, she’s often still working.
“We’re on all the time, because there’s no other us,” Waldron said. “When people do leave employment, it’s usually because they are overworked.”
The root of the funding problem
A primary reason local Indiana health departments are poorly and inequitably funded is because on average more than 70% of their funding comes from county governments, whereas on average nationally, most local health departments only receive about 25% of their funding from local governments. Other funding comes from federal direct or pass-through payments, state dollars and services and fees.
St. Joseph County health officer Robert Einterz called the current system, with its lack of centralization, “completely dysfunctional.”
That means health departments are funded based on what local elected officials deem is most important, most of whom don’t have health expertise and some of whom are distrustful of some public health initiatives following the COVID-19 pandemic.
“Those counties have to use that [money] to address their court system, their jails, their roads and other things,” Box said. “There’s just oftentimes not really much money left to be able to invest in local public health.”

Sometimes elected leaders are also either reluctant to apply for federal grants, because they either don’t want the federal government involved in local government or because they don’t want to be stuck with the bill after the grant ends, health officials say.
In other cases, there is a classic chicken and the egg conflict. Because local health departments don’t have the resources to hire someone dedicated to evaluating federal grants, they don’t apply for certain time-consuming grants in order to get more resources.
Similarly the health department in Hendricks County missed out on a grant for an infant mortality review team because they didn’t have physical space for another employee, said Michael Aviah, a public health education specialist in the county.
Counties such as Hendricks have succeeded in part because it’s created partnerships with local nonprofits or hospitals, which enables it to complete health assessments and act on those results. But coordinating those partnerships takes resources, too. Hendricks County has a position dedicated to partnerships.
When a local health department has one person handling all environmental complaints, there just isn’t the staffing to dedicate to forging those relationships.
“There’s definitely a lot of energy and time and resources that goes into building and establishing those relationships,” Aviah said. “I could definitely see that being a barrier if you don’t have the capacity to do that.”
Rural counties feel the pinch
The problems caused by a shortage of funding is exacerbated in rural communities where county officials are forced to choose what to do with a smaller pool of money.
Owen County’s health department, for example, was among the lowest-funded health departments in the state per capita pre-pandemic. The rural county, which sits between Bloomington and Terre Haute, currently only has three full time positions and one part-time position in its health department, in addition to four contract employees funded by temporary grants that will all eventually end.
There’s plenty of services Christina McBride, the county’s health administrator and vital registrar, would like to provide if the department was provided more money, such as offering transportation to doctor appointments, providing physicals or even simply investigating and cleaning up more unsanitary, rodent-attracting trash complaint sites. The majority of doctors in the county are located in just one town within a two-mile area, and there’s no public transportation.
But the county of roughly only 21,000 people has a limited budget, about 1/17th the size of Marion County’s.
“This county is poor,” McBride said. “They’re in a financial bind all the time, so they’re not going to be willing to give us any extra.”
As of 2021, counties reported having a median of seven full-time health department employees, ranging anywhere from zero full time employees in 10,000-resident Martin County to 940 in Marion County. That means county employees are forced to take on multiple roles, sometimes without adequate training.
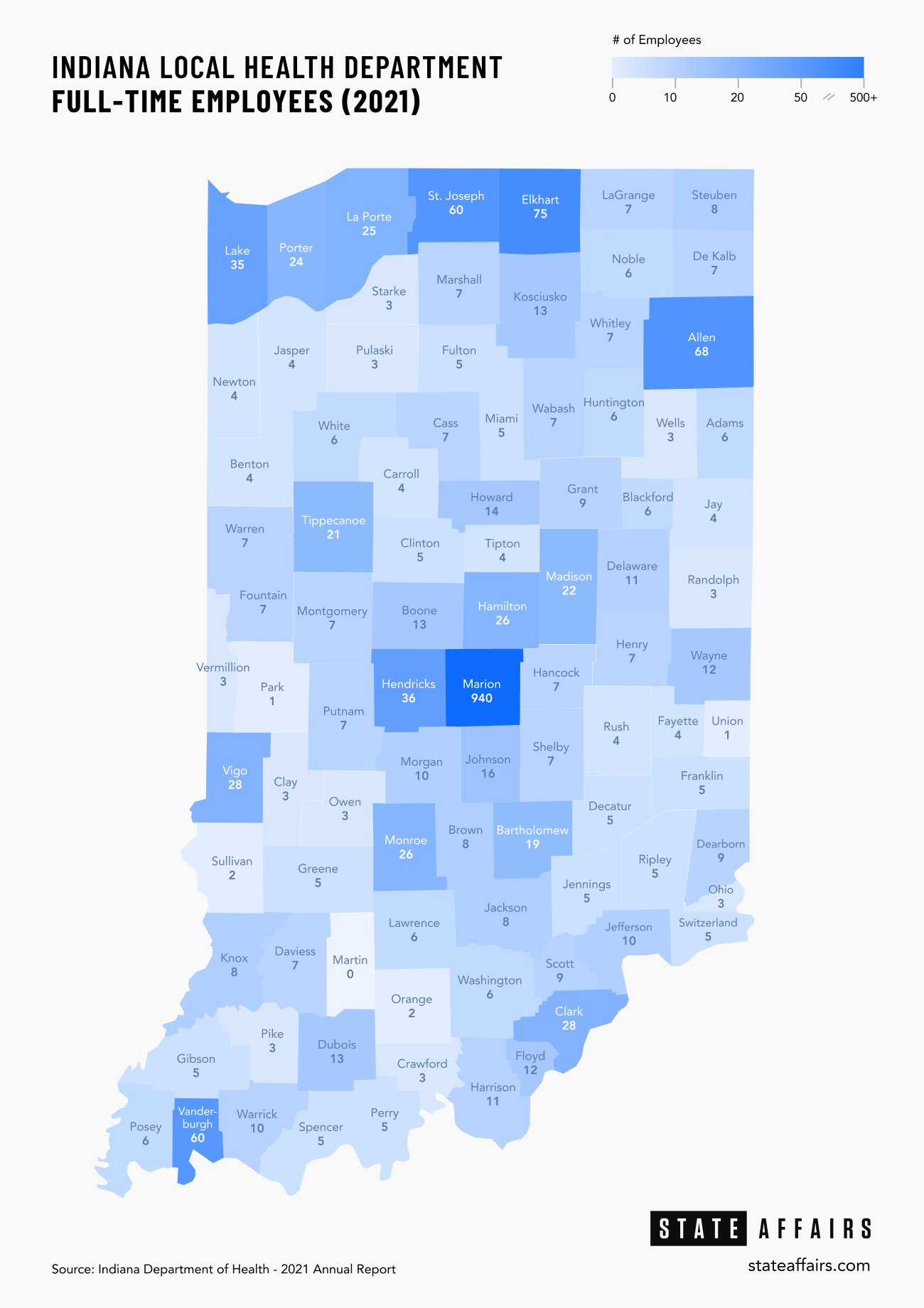
It also means that if an employee gets injured, sick or quits, communities are put in a bind and have to either rely on other cash-strapped health departments to lend a hand or temporarily stop providing the service.
In Ripley County, a rural community near Cincinnati with fewer than 30,000 people, the health department was forced to struggle with a staffing shortage after the person responsible for inspections of new construction quit, said Dr. David Welsh, the county’s health officer. That delayed permits on new construction for buildings and homes for weeks while the county looked for a backfill, despite some help from other communities and the state.
Welsh, and multiple other health officials, also expressed concerns about a lack of data available to counties, as well as the ability to analyze that data. Currently, schools in his community are dealing with high absentee rates. He’d like to know about disease upticks and be able to warn schools before it starts impacting school attendance.
“I’d like to get a heads up that the horse is trying to break out of the barn before it’s out of the barn and down the road,” Welsh said, “and that comes from acquiring data and analysis of data.”
Even in some larger counties, such as St. Joseph County, the lack of data is problematic. Einterz, the county’s health officer, emphasized that he’d like to be able to get a handle on why some people aren’t getting regular cancer screenings. That’s data he just doesn’t have.
The Solution
For the governor's Public Health Commission, the solution begins with an infusion of cash to each county health department. The commission asked state lawmakers to set aside an additional $243 million each year in this upcoming budget cycle.
Even with the weight of Gov. Eric Holcomb himself behind the Health Commission as well as that of Luke Kenley, a former influential senator who co-chaired the commission, getting support from a majority of lawmakers, including those who lead the budget-writing process, will be challenging.
“Even though the pandemic has put the spotlight on healthcare, we never had, during the entire time I was in the legislature, any kind of comprehensive review of the public health program,” Kenley said. “It’s like a brand new subject almost, and anytime you get into a new subject, then you’ve got to go back to ground zero and explain a lot of basics and get people up to speed.”

Budget writers are grappling with countless other budget requests this cycle, such as more education or mental health funding. There’s only so much to go around in a Republican state legislature dedicated to maintaining significant reserves and lowering taxes, amid concerns about inflation eating up any extra revenue.
Senate President Pro Tempore Rodric Bray said last month that he couldn’t see the legislature spending the combined $480 million in the next two-year budget that’s being requested for public health.
“I think it might be difficult,” Bray said. “That’s a big bite.”
But health advocates point to other large dollar numbers: The extra costs associated with health problems in Indiana that could have been prevented.
Chronic diseases, for example, directly and indirectly cost $75.5 billion in Indiana each year, and smoking results in $3 billion in annual healthcare costs for Indiana, according to the Public Health Commission’s report.

Sen. Ed Charbonneau, chair of the Senate Health and Provider Services Committee, is hopeful he and other health advocates will be able to get the total requested funding in at least the second year of the budget.
The Valparaiso Republican is carrying the health commission’s bill this upcoming legislative session, which starts in January. In addition to providing extra funding for county health departments, his bill would create regional districts that would better allow the state health department to communicate and pass resources onto individual health departments.
He knows the funding specifically is a hard sell. Complicating the issue: Changing health outcomes won’t happen overnight even if funding is poured into the system.
“A big issue we’re going to have to deal with is education of the public and I think the legislators, about where we are, why this is important,” Charbonneau said. “One of the primary things for me going forward is changing the focus from treatment to prevention.”
It’s been about eight years since the HIV outbreak swept through Scott County. More than 200 people were infected, but health officials were eventually able to stem the tide, thanks largely to the help of a clinic offering syringe exchanges, information on recovery resources and, of course, HIV testing.
But in at least 60 other counties? HIV testing provided by local health departments remains out of reach, according to the health department’s 2021 report.
Some told State Affairs they don’t have the resources to offer it.
“There’s a dire need for it because a lot of people don’t know where they can get tested,” said Aviah, whose county no longer provides HIV testing. “It’s really important that we, the health departments, are able to provide that.”
Twitter @STATEAFFAIRSGA
Facebook @STATEAFFAIRSUS
LinkedIn @STATEAFFAIRS
Contact Kaitlin Lange on Twitter @kaitlin_lange or email her at [email protected].
Header photo: (Credit: Centers for Disease Control)
Read this story for free.
Create AccountRead this story for free
By submitting your information, you agree to the Terms of Service and acknowledge our Privacy Policy.
Who is Jamie Reitenour? Indianapolis mom mobilized volunteers to make governor’s ballot
EDITOR’S NOTE: This is one in a series of profiles of the candidates running for Indiana governor.
ZIONSVILLE, Ind. — It wasn’t the largest campaign event the 2024 election cycle is likely to see.
About 15 people, some of them children, gathered on a rainy April night at Our Place Coffee, nestled just feet from the watchful eye of Zionsville’s Abraham Lincoln mural. But Republican gubernatorial candidate Jamie Reitenour, an Indianapolis mom with no previous political experience, spoke with every single one of them.
It was one part coffee-and-issues politicking and one part informal Bible study, complete with scripture quiz questions for the kids in attendance.
Reitenour, well-worn Bible in hand, shared her oft-repeated story of being called by God to run for governor about six years ago — a destiny confirmed by friends and strangers alike along the way, she said. This charge, she told the group, would allow her to rise above traditional campaign currency, such as fundraising dollars and polling numbers.
Suzanne and Shon Hough sponsored the event after meeting Reitenour at their shared church, Horizon Christian Fellowship in Lawrence.
“As soon as we met her, we knew this is someone to support,” Suzanne Hough said. “We knew she wasn’t a politician. She was called. She has a love and compassion for people.”
That is how Reitenour has made it this far — how she gathered the 4,500 state-mandated signatures to qualify for the May 7 primary ballot, how she’s made it onto a stage filled with more experienced and wealthier opponents. For more than a year, she’s hosted several small events per week throughout the state, traveling some 35,000 miles, by her count.
The dozen or so latte-sipping supporters had a part to play, the candidate said.
“Go to your contact lists and tell them about our Facebook,” Reitenour said. “We could reach 144 people today if we all did that.”
The call
Reitenour’s purpose changed in 2017 while walking through downtown Indianapolis with her husband, Nathan.
“I just heard a whisper: You’re going to be the governor of Indiana,” Reitenour told State Affairs.
The couple wandered over to the governor’s mansion.
“We looked at it and thought, ‘That does not look like our family,’” she recalled. “So I just put the calling on the shelf.”
Indiana requires gubernatorial candidates to have lived in the state for at least five years. She had only just moved from Michigan.
Reitenour believed the country was in a good spot under then-President Donald Trump. Why would she need to run?
“I just thought about it,” Reitenour said. “Why would the Lord call an ordinary person to something like that when the nation was doing so well? But the reality of scripture is that you see these times where people are called, and you can see the reasons for the calling around them.”
Her regular Bible contemplation soon took her to the Book of Nehemiah, who was a governor. Another sign, she said.
The state’s response to the COVID-19 pandemic set off alarm bells for Reitenour, who considered steps like mask requirements an affront to personal liberty. She brings up the subject often, and it made it into her coffeehouse remarks.
“How am I in a conservative state, but I don’t feel free?” she told the crowd.

After COVID-19 and the election of President Joe Biden, Reitenour began to think more seriously about running for governor.
Her mission was affirmed first by a close friend, whom Reitenour said received a similar calling from God to help her candidacy, and then by strangers, whom she said confirmed her destiny during separate chance meetings at a Panera Bread location.
She began to meet with church groups and advocacy organizations that align with her views, including Moms for Liberty and Indiana Right to Life. Despite being referred to as an activist on the campaign trail, Reitenour said she is not part of any activism group.
Getting on the ballot
This network of like-minded supporters would soon serve as the volunteer arm of Reitenour’s campaign.
Indiana requires candidates for governor to collect at least 4,500 signatures from voters, including at least 500 from each of the state’s nine congressional districts. It’s a tall order even for seasoned politicians, who often hire specialized operatives for the task.
“The mystery of how we did that will also be the mystery of how we win,” Reitenour said.
She focused on growing supporters and gathering signatures at each small event she hosted, then mobilizing those attendees to gather still more for her.
“I had a formula in my heart for this that the Lord gave me at 4 a.m. one morning,” she said.
The campaign
Reitenour made the ballot, but she is the least-known candidate in a field that includes Sen. Mike Braun, Lt. Gov. Suzanne Crouch, former state Attorney General Curtis Hill, former state Secretary of Commerce Brad Chambers and Eric Doden, a Fort Wayne businessman and previous president of the Indiana Economic Development Corp.
She has no previous political experience. She is a stay-at-home mom who also homeschools her five children and volunteers through ministry. Her previous work experience includes compliance management at a mortgage company, secretarial work and even a stint as an assistant coach in women’s field hockey.
Reitenour was selected in the governor’s race by just 2% of respondents in a recent State Affairs/Howey Politics Indiana poll, tying her with Hill for last place behind front-runner Braun (44%). She has consistently polled in the low single digits.
While other gubernatorial candidates can draw from years of campaign fundraising experience or millions in personal finances, Reitenour had raised just a little more than $54,000 as of March 31.
She has thus found herself paddling in a proverbial ocean of campaign spending.
The four top-polling candidates — Braun, Chambers, Doden and Crouch — have spent a combined $20 million.
After participating in the first gubernatorial debate on March 11, Reitenour did not qualify for a March 27 debate hosted by WISH-TV due to her fundraising numbers, as the television station required candidates to have raised $300,000 by December.
She was also excluded from a March 26 Fox59/CBS4 debate for not reaching a 5% polling threshold. She will be included in the final April 23 debate, hosted by the Indiana Debate Commission.
Reitenour has campaigned using a constantly shuffling group of volunteers. She has only one full-time employee: campaign assistant Casey Pierce, who met Reitenour through his mother’s church.
“It just felt like the right thing to do,” Pierce said of joining the campaign. He has never worked in politics before.
Pierce called his initial meeting with Reitenour “a Holy Spirit encounter.”
Reitenour’s platform
Reitenour described education as the state’s “greatest vulnerability,” and thus her primary platform.
“The next generation is not being educated well, and this has been a long time coming,” Reitenour said.
She has received guidance from the Hamilton County chapter of Moms for Liberty, which made national headlines in 2023 after using a quote attributed to Adolf Hitler in its first newsletter. The nonprofit, which pushes against socially minded education reforms like critical race theory, subsequently apologized.
Reitenour likewise opposes ideas like social-emotional learning in classrooms. Her plan also proposes removing technology from grades K-5, calling for private businesses to sponsor classrooms and requiring all students to pursue an apprenticeship before high school graduation.
She also favors an audit of the Indiana Economic Development Corp., tax cuts, a focus on investing in small towns and generally “pointing Indiana in the direction of family.”
The future
At her coffee shop appearance, Reitenour shied away from admitting her long odds in the race.
“The political system is meant to squeeze people out, but I am working against it,” she said.
She pledged to continue organizing no matter the primary election results.

About Reitenour
- Age: 44
- Hometown: Indianapolis
- Education: Psychology degree from Missouri State University
- Family: Married to Nathan Reitenour, with five children, ages 13, 11, 10, 9 and 4
- Job: Stay-at-home mom, homeschool teacher
- Work history: Former compliance manager at Windsor Capital Mortgage, former athletic director at Calvary Christian School (at Calvary Chapel Vista church in California)
Read these related stories
- Eric Doden is running from behind but hopes his ‘bold vision’ will propel him forward
- Suzanne Crouch positions herself as a ‘different’ candidate for the voiceless
Contact Rory Appleton on X at @roryehappleton or email him at [email protected].
And subscribe to State Affairs so you do not miss an update.
Facebook @stateaffairsin
Instagram @stateaffairsin
LinkedIn @stateaffairs
Child care: Where Republican candidates for governor stand
Six candidates are seeking the Republican nomination for Indiana governor in the May 7 primary. State Affairs is providing looks at their stances on several issues. Jennifer McCormick is unopposed for the Democratic nomination.
Indiana’s high cost of child care ranks as a primary concern for many of the state’s families.
According to Child Care Aware of America, a nonprofit organization that studies child care costs, Indiana ranks as the eighth most expensive state for infant and toddler care. The cost for caring for a baby averages 14.5% of a family’s median income, while toddler care is 12.9%.
Only 5% of Indiana families can afford infant care, the Economic Policy Institute found.
State Affairs asked each of the six Republicans vying for Indiana governor — U.S. Sen. Mike Braun, former state Secretary of Commerce Brad Chambers, Lt. Gov. Suzanne Crouch, Fort Wayne businessman Eric Doden, former state Attorney General Curtis Hill and Indianapolis mother Jamie Reitenour — how they would lower Indiana families’ child care costs if elected.
Here are their responses.

Mike Braun
“The high cost of child care burdens Hoosier families and businesses, who are trying to recruit and retain the best workers. As governor, I am open to and will work on solutions that will reduce the cost of child care, which is a win for our economy and families.”

Brad Chambers
“As governor, I’ll explore strategic expansions of all-day pre-K for 3- and 4-year-olds, including potentially increasing the income eligibility level for state-funded pre-K programs. I’ll create a state-level child care tax credit that requires recipients to work to be eligible to receive it.”
Chambers said he would also explore incentives for employer-sponsored child care.

Suzanne Crouch
“First, I would lead the effort to eliminate the state’s individual income tax, which will mean more money in families’ pockets and help reduce the financial strain of child care expenses … As governor, I would propose that the General Assembly put a priority on early childhood education throughout Indiana.”
Crouch would also support the expansion of at-home and religious-based child care, she said, noting Indiana has “some of the highest relative child care costs in the country.”

Eric Doden
“I’ve offered a bold plan to expand pre-K access to every community in the state. By partnering with communities, nonprofits and education partners, we will begin addressing this important need. … We need a state with thriving communities and access to opportunity. Cost of child care concerns are downstream of family formation rates, good-paying jobs, home ownership and a host of other economic and community issues.”

Curtis Hill
“The government is not responsible for providing child care for private sector employees. Its responsibility is to dismantle the licensing and regulatory burden that prohibits new child care providers from entering the market. If we want to lower the cost of child care, we must cut the government regulations forcing child care facilities to either close or raise prices to meet unnecessary government requirements.”

Jamie Reitenour
“We cannot bear down on taxpayers for everything. We just cannot do it. But we can talk to the private sector and reason together. Can we have in-house day cares at offices? Yes. Can we have employers operate growth centers for employees’ kids? Yes. Taxpayers are not the answer; the private sector is. With competition for qualified workers, larger businesses already employ creative benefits, including child care assistance, to attract talent.”
Read these related stories:
Contact Rory Appleton on X at @roryehappleton or email him at [email protected].
And subscribe to State Affairs so you do not miss an update.
Facebook @stateaffairsin
Poll finds Holcomb popular among Republicans even as potential successors keep distance
Indiana Gov. Eric Holcomb remains popular among Republicans, according to a State Affairs/Howey Politics Indiana poll, even as the GOP candidates to take his place have kept their political distance from him. The polling results released Thursday show Holcomb with an overall positive job-approval rating of 69% among self-identified Republicans and Republican-leaning independents. The results …
‘It’s sort of a blowout’: Braun holds commanding lead in ‘State Affairs/Howey Politics Indiana’ poll
U.S. Sen. Mike Braun holds a commanding lead in a new State Affairs/Howey Politics Indiana poll of likely Hoosier Republican voters in the May 7 gubernatorial primary. Asked who they would vote for if the primary were held today, 44% of respondents picked Braun. Lt. Gov. Suzanne Crouch trailed with 10% of the vote, and …




